By LISA EISENHAUER
June 25, 2020
Pamela Mitchell-Boyd remembers exactly when the breadth of the racial disparities of the coronavirus pandemic hit her full bore.

Mitchell-Boyd
It was April 6 and she was listening to a press conference on the coronavirus by Chicago Mayor Lori Lightfoot. Among the statistics the mayor cited, Mitchell-Boyd recalls, was that more than half of the Chicagoans who had tested positive for COVID-19 and 72% of those who had died from the virus were black, and that's in a city where African Americans make up 30% of the population.
"When these numbers presented themselves it just became astounding and I knew that our health system needed to address our patient population and understand how the disease was affecting the people that we care for," said Mitchell-Boyd, system director of diversity, inclusion and language services for Ascension's AMITA Health.

Ikedrick Williams is discharged in April from AMITA Health Adventist Medical Center Bolingbrook in suburban Chicago to the delight of his family. He recovered from a severe bout with COVID-19.
She reached out to colleagues within the Chicago-based system. They quickly set up a team with executives, advocacy leaders, and analytics and research specialists to compile demographic data from AMITA's 19 hospitals and 200 other care facilities about patients who had tested positive for the coronavirus. The team hopes to use data on case and death characteristics to help the system identify populations in the communities it serves who are most vulnerable to severe outcomes from the infection and improve their access to testing, care and services.
"We're in the process of trying to figure out what communities we can be the most helpful to in improving some of these results," Mitchell-Boyd said.
Breaking down the numbersA
report posted in early April by the Centers for Disease Control and Prevention found that of people hospitalized for COVID-19 whose race was known, 33% were black. U.S. census data says black Americans make up about 13.4% of the population. At the time race and ethnicity was missing or not specified for nearly two out of three COVID-19 cases reported to the CDC.
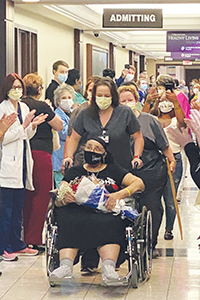
Martha Simmons, the first COVID-19 patient admitted to CHRISTUS Ochsner St. Patrick Hospital in Lake Charles, Louisiana, is discharged with a celebration on June 12 having spent almost three months in the hospital. The pandemic has taken an especially harsh toll on African Americans.
An analysis published by the Kaiser Family Foundation on April 21 pooled CDC racial and ethnic data on COVID-19 with state reported data to reach the same conclusion: the virus was disproportionately affecting communities of color. The Kaiser report said that in six states Hispanics were overrepresented among those confirmed to have gotten the virus. The foundation said underlying health, economic and social issues made communities of color more vulnerable to the pandemic.
A few days before the CDC report posted, seven physicians organizations led by the American Medical Association urged the U.S. Department of Health and Human Services to collect, analyze, and make available standardized data. The association said that data should include race, ethnicity, and preferred spoken and written language related to the testing status, hospitalization, and mortality associated with COVID-19. "These data are essential to understanding the unique challenges and inequities facing communities of color and individuals with Limited English Proficiency," the organizations wrote to HHS Secretary Alex Azar.
"While COVID-19 has not created the circumstances that have brought about health inequities, it has and will continue to severely exacerbate existing and alarming social inequities along racial and ethnic lines, e.g., in housing stability, in employment status, in health care access, and in food security," the physicians groups wrote.
Demographic data mandate
On June 4, HHS issued guidance to laboratories doing COVID-19 testing that requires them to collect demographic data for patients that includes race and ethnicity and submit that information along with test results.
CHA supports legislation to improve the collection of racial and ethnic data related to those who have contracted COVID-19. The association also is pressing Congress and the administration to provide additional funding and policy support for outreach, testing and treatment in communities of color and additional resources for vulnerable communities suffering the economic consequences of the pandemic to address social needs such as homelessness, housing and rental assistance, and food assistance.

Ross
Speaking May 7 during a podcast hosted by CHA, Dr. Sam Ross, chief community health officer for Bon Secours Mercy Health, said the statistics showing the disproportionate racial impact of the virus are not surprising. Ross said the numbers spotlight racial disparities in health care that existed before the pandemic.
"The real issue now is not that it's occurring and being highlighted, but what are we going to do about it," he said. "We've been talking about these issues of inequities for now decades."
What needs to be done, in Ross' view, is for health systems to develop trust among communities of color by bringing them to the table when programs, policies and services are taking shape. "If we start to behave in a way that is really about engaging and including, then I think that will go toward building trust and us understanding whether or not what we're doing is really the right intervention," he said.
Action, advocacy
Rosalyn Carpenter, senior vice president and chief diversity officer for CommonSpirit Health, said caring for underserved communities and addressing racial disparities is at the core of the health system's mission.

Carpenter
CommonSpirit is addressing COVID-19 disparities in part by providing free virtual urgent care visits for anyone experiencing mild to moderate symptoms of the illness, Carpenter said. For all COVID-19 patients, it has suspended billing until cost-sharing between government and insurers is sorted out.
The health system also is advocating for government assistance packages to include the heavily minority service workforce that has had to remain on the job amid the pandemic, Carpenter said. In addition to financial help, she said, the workers need on-the-job protections to keep them safe from contagion and they need to have access to testing, and health care services if they contract the virus.
"We need smart policies and massive financial assistance packages that enable people to continue to be safe," she said.
Carpenter noted that many of the people who have had the worst outcomes from COVID-19 have preexisting conditions, such as high blood pressure, stroke, diabetes, cancer or asthma. Those are conditions that disproportionately afflict people of color. And she said research has shown that those higher rates of chronic disease are driven by socioeconomic factors, such as lack of access to health care, unemployment and underemployment, poor access to nutritious food and inadequate housing.
"We know that if we work to address those social determinants of health, ultimately we will improve the health of those individuals — be they vulnerable, be they people of color — wherever they live," she said.
Localizing disparities
Providence St. Joseph Health is breaking down data related to COVID-19 from its 5 million patients geographically and sharing it with local ministries so they can use it to identify the most vulnerable people in their communities, said Dr. Rhonda Medows, the system's president of population health management. "We want them to actually do more outreach, do more frequent calls, more check-ins with the complex populations after we've expanded who it is that they're looking at," she said.
Medows
Providence's medical record system already was integrated with a social services platform called Community Pathways to Health — the system has functionality that merges COVID-19 incidence rates with details about patient needs. That information informs local health ministries about what social services are needed by the vulnerable groups and helps them decide how best to partner with agencies and nonprofits in their communities to set up things like food banks to address those needs.
In addition, Medows said, Providence is ramping up efforts to assess patients for Medicaid eligibility and to help those who qualify to enroll. It's also working with companies that make its virtual tools, such as smartphone apps, to ensure that those tools are in languages and formats that make them easy to use.
"These are all things that are in progress," Medows said. "Showing people the data goes a long way in explaining why it's important."
Seizing an opportunity
Like other health systems, Providence has been advocating for COVID-19 testing and treatment for high-risk populations, but Medows said the system doesn't plan to stop there. It will be urging that those patients be given access to potential treatments such as the drug remdesivir, which studies suggest can lessen the virus' impact in some patients. And, should a vaccine for the virus be developed, she said she and others with the system will be champions for its use first among those populations that have been hit hardest.
"We always say that out of adversity comes opportunity," Medows said. "This is an opportunity to help a lot of people who historically have not received the aid they need."