By LISA EISENHAUER
The social teachings the Catholic health ministry is founded on create a special responsibility for Catholic health care providers to partner with and advocate on behalf of the public health sector in the view of Mike Slubowski, president and chief executive of Trinity Health.

Slubowski
Slubowski points out that the ministry's mission includes reaching and serving the most vulnerable and improving the health of its communities. "We at Trinity think a strong public health infrastructure is essential to building a health care system that can ensure access to high-quality care for all and to public policies that advocate and advance the common good," he says.
Part of Trinity Health's advocacy agenda is calling for more funding and support for the public health sector at the federal, state and local levels. Similar advocacy efforts are underway at other large Catholic health systems, including Providence St. Joseph Health, and at CHA.
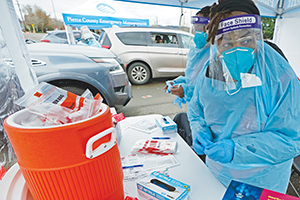
Medical assistants at a drive-up COVID-19 testing clinic in Puyallup, Washington, near Seattle, fill a cooler with nose swab samples that will be sent to a lab. People using the testing site on Jan. 4 faced waits of several hours. The site was run by the Pierce County Department of Emergency Management. The resources of public health agencies have been stretched thin by the pandemic and many public health officials have taken the brunt of criticism over the nation's response to the crisis.
Ted S. Warren/Associated Press
The health systems and CHA all see public health officials and agencies as central to ensuring that communities have access to disease testing, vaccines and other basic health services and that the nation is prepared for health emergencies such as future pandemics and environmental catastrophes. They say the crisis created by COVID-19 shined a spotlight on how vital a strong public health infrastructure is to the nation.
In addition to news reports of public health agencies being overwhelmed and undersupplied during the pandemic, there have been many reports of public health officials being threatened by members of the public, or being fired or having their authority reduced by officials critical of lockdowns and masking requirements. Many public health officials resigned or retired.
Kaiser Health News in 2020 described the public health care workforce as being "under assault when it's needed most." Meanwhile, a study by the Robert Wood Johnson Foundation and Harvard T.H. Chan School of Public Health released last May found strong support among the public for more federal spending for public health while also finding the positive ratings of the public health system had declined from 43% in 2009 to 34% in 2021.
The Centers for Disease Control and Prevention, the nation's public health agency, has been buffeted by the political divisions in the country's COVID response since the start of the pandemic. It's been criticized for confusing and shifting guidance and for a lack of independent guidance. In a January telebriefing with reporters, CDC Director Rochelle Walensky promised to improve communications.
Underinvestment feeds inequity
Trinity Health put its case for assisting the public health sector into a position paper it issued last year called "Care for the Common Good" and subtitled "Our COVID-19 Journey." It notes that, "following years of underfunding and lack of prioritization, America's public health infrastructure was ill equipped to address the COVID-19 pandemic. COVID-19 has clearly illustrated how this underinvestment is contributing to inequities within our health care system and society."
Slubowski discussed the roles the public and private care sectors have played in addressing the pandemic in an American Hospital Association podcast last summer with Dr. Rod Hochman, president and chief executive of Providence St. Joseph Health. At the time of the recording Hochman chaired the AHA board. Both men are past chairs of the CHA Board of Trustees. In the podcast, Slubowski says Trinity Health and other health care providers "have become the de facto public health system during this crisis."

The community vaccination site at the Lumen Field Event Center in Seattle opened in March 2021 as a collaboration between the city of Seattle, stadium operator First & Goal Inc. and Swedish Health Services, an affiliate of Providence St. Joseph Health. Before the site closed in June, workers there gave tens of thousands of COVID-19 vaccinations.
In the podcast and in a recent interview with Catholic Health World, he shared many instances during the pandemic when his system has taken on responsibilities across the communities it serves that the public health sector didn't have the resources or the coordination among the various agencies and officials to handle.
Examples he gave included Trinity Health's having to secure and distribute scarce supplies and medications across its 25-state service area, educate the general public about how to reduce infection risk, run public testing and vaccination sites including in locales where infection rates were especially high, and linking people with unmet needs to social service providers.
Suggestions for change
Trinity Health's position paper urges policymakers to provide more funding and authority for public health officials to take on health care supply chain coordination in times of acute shortage, be a health care information hub for providers and take the lead in health education and efforts to stem the spread of contagious disease. Among its suggestions are that the public health sector have computer systems that allow for the exchange of information with health systems and care providers; that it offer guidance on practices across all three levels of government; and that it provide more training, education and subsidies to bolster the health care workforce.
Slubowski says the public-private health care partnership needs to work in both directions. "I think the public sector definitely relies on us to be a backstop for many efforts, but we also have to have a coordinated approach to communication, to resource allocation, to distribution of care across our communities instead of leaving it all in the hands of the health systems to figure out among themselves," he says.

Bombard
Jacquelyn Bombard, executive director of federal relations at Providence St. Joseph Health, says a solid public health sector is vital to advancing some of the system's primary goals. "One priority of Providence's is achieving health equity and we firmly believe that we can't achieve health equity if there's instability within the public health infrastructure," she says.
Public health furthers the push for equity in a number of ways in Providence's view. That includes by seeing that everyone has access to health education, medication and quality care.
All hands on deck
Bombard says Providence also considers a strong public health sector as essential to the system's pledge to address climate change and the harsh toll environmental degradation takes on vulnerable communities. Environmental issues such as polluted air and drinking water have a direct impact on population health. Protecting air and water resources requires oversight and action by lawmakers, regulators and public health officials, she notes.

A worker moves supplies at a Trinity Health's 500,000-square-foot warehouse in Fort Wayne, Indiana. Trinity Health's top executive says his system, like others, have taken on responsibility for distributing supplies such as personal protective equipment and scarce medications across communities because public health officials have at times been unable to mount a sufficient response.
Providence also is advocating for funding increases so public health officials and agencies can do more data collection on health issues, coordinate emergency response training within and across communities and provide more testing and treatment for infectious diseases and chronic conditions to underserved communities, especially those in rural areas where public health services are sometimes the only health care available.
"Right now, it's been all hands on deck working with public health officials on our COVID response, but we hope that we can get to a place to be more proactive to really strengthen our partnerships," Bombard says.
Federal efforts
Paulo Pontemayor, a CHA director of federal government relations, says CHA advocates in Congress for increased funding to strengthen the public health sector.

Pontemayor
"We've made public health, especially in the last two years with this pandemic, a big priority knowing full well that a lot of our members have to depend on their state, county and city public health departments to work together to combat COVID-19," he says.
CHA applauded the passage last year of the American Rescue Plan. The Biden administration said that federal legislation, which CHA advocated for, includes $7.4 billion to recruit, hire and train tens of thousands of public health workers. The U.S. Department of Health and Human Services has earmarked $80 million to build up the U.S. public health informatics and data science workforce — particularly by training students from underrepresented minorities in data science as a way to strengthen analysis around race and ethnicity-specific public health data. The goal is to harvest and refine data at the local and state level to improve health equity in future public health responses.
However, Pontemayor says much more is needed. "We know that that was just really a down payment," he says of the American Rescue Plan. "We know that over the years public health has really not been funded as robustly as other federal programs."
CHA supports the Build Back Better legislation that the Biden administration is struggling to guide through Congress. The measure includes additional programs and funding streams to give local public health officials tools to prepare for the next pandemic and to address racial and ethnic disparities in care, especially as they relate to maternal health, behavioral health and substance abuse, Pontemayor says.
Trinity's coordinated response
At the onset of the pandemic, Trinity Health activated a systemwide incident command structure that morphed into the framework it uses to address the exigencies of a health crisis now entering its third year. Trinity Health created a systemwide structure to ensure that staffing, supplies and other resources are in place at its facilities as needed and that protocols and best practices are shared across the system in a timely way.
"We have a national team that focuses on all of the big issues and then we have COVID response teams in every state and they are totally aligned with what we're doing nationally," Slubowski says.
The coordinated effort has functioned well, he says, even in the face of differing public policies and public health structures across the 25 states and hundreds of cities that Trinity Health serves.
The structure could potentially be a model for the public sector, Slubowski says. "I think public health is something that's definitely got to have a national set of principles and approaches and guidance," he adds.