
Mitchell
By JULIE MINDA
When Cory Mitchell joined Mercy Health Muskegon as director of mission integration in March, he stepped to the helm of a department that would soon face its biggest challenge ever. Mitchell spoke with Catholic Health World Associate Editor Julie Minda about what it's been like for him and his staff of 19 chaplains to tend to the spiritual well-being of patients and nearly 4,700 staff and physicians at three hospital campuses and at a network of outpatient sites in the Muskegon, Michigan, area in the throes of the pandemic that has overwhelmed available resources and taxed human endurance.
With coronavirus infections spiking to the highest point yet this fall in Michigan and Muskegon County seeing one of the biggest surges in the state, the pressures on exhausted staff continue to mount. In mid-November, Mercy Health Muskegon opened additional COVID care beds at its Hackley campus. That campus had closed to inpatient care in October as part of thepr final phase of renovation and construction at Mercy Health Muskegon's main campus.
When the pandemic first started in the spring, we averaged about 10-15 COVID cases per day in our 300-bed facility, which is our Mercy campus. And that count had been about flat. Then in October and November, the numbers took off like a rocket and we just had a high of 152 COVID cases (at the start of December). We're projected to increase to a census of 200 COVID cases. It's been an exponential growth of cases.
To keep in touch with staff, and to understand how they are faring under these conditions, our department chaplains and I have been rounding on the floors throughout the pandemic, as has our facility leadership.
We have over 100 colleagues right now who are COVID-positive. People are worried about their family members, their colleagues and themselves. They're worried about childcare.
At the start of the pandemic, our COVID patients were on the sixth floor and at that time we were seeing a death in that unit every few days, which was a big number for them. It was hard for them, but staff were coping. They were saying, "I will be fine. I can get by."
But now it's been months and the numbers of COVID admissions have gone up. You go through the floors and you look at the nurses and you see that 1,000-yard stare. I'm a vet and looking at them reminds me of the look I've seen on soldiers in the VA who have post-traumatic stress disorder. This 1,000-yard stare is a severe form, and it happens when people become disconnected from what's going on around them. When this happens to our clinicians, it can lead to depersonalization of care, which can jeopardize patient care.
We know that COVID is a bio-psycho-social-spiritual phenomenon and so to treat it we need to bring bio-psycho-social-spiritual resources to bear – for colleagues, for patients, and for the community. While I do not have the experience in the other areas, I can facilitate these groups getting the help they need from a social and spiritual perspective.
Two months ago, the mission department started virtual "sounding rounds" for staff. With the sounding rounds, we are plumbing the depths of being a human being in health care. We bring the good, the bad and the ugly to bear, about being fully human.
The senior manager of spiritual care and a clinician are empowering employees through resiliency rounding. They're looking for warning signals and they are looking at how they can make things better for colleagues. We've developed a warning signals worksheet so people can understand the symptoms of burnout and know what action steps to take when they detect burnout in themselves or others. We tell them what resources they can use. We are distributing the information in our newsletters for managers and colleagues. We're normalizing seeking help.
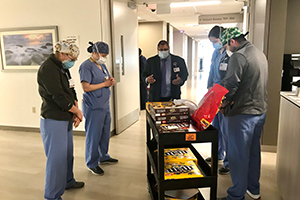
While rounding with a candy cart, Cory Mitchell, Mercy Health Muskegon’s director of mission integration leads a prayer. Mitchell says he always asks staff what they want to pray about because doing so opens a window on their deepest needs and fears.
And something new we're doing in response to the pandemic is "Wednesdays at the Well." This is a Liturgy that we have at 8 a.m. on Wednesdays. We have music and people are fed by the word, by reflections and by prayer and by being together. This helps to pull them away from their work when they need that time away. We have a PowerPoint we play and the first slide is on colleague resources – financial support, the spiritual care pager number. I encourage them to use all of these resources, and we must keep repeating the invitation to seek help because it is not normal for health care workers to seek help. We have to make sure that we are nonpunitive and that we don't stigmatize, so that people will seek help.
It is critical that we see staff – in-person, when we can — so we know how they are doing. Also, when we pray with them, including during our rounding, we can engage with them. Prayer can be an anchor. When I and other chaplains are rounding, we ask people what they want us to pray with them about and often this is when they will articulate their deepest needs and their most profound fears. We also have an anonymous, virtual prayer request form. So, many colleagues will share their prayer requests that way too. Praying about these concerns is a great way, an unguarded way, to articulate needs.
The rounding and other approaches have been a tremendous hit with staff. And, when the smiles appear and the faces brighten as we're talking, we feel there's been progress. Every day, we're getting positive feedback.
Health care worker burnout is an issue of national importance. It affects our ability to recruit and retain our workers. We need to support our colleagues, including ones who may be forgotten and the least paid, like the environmental services team members.
There are multiple strains on our staff now and we have to be attentive to the staff members. I think that when colleagues are not performing at their best, patient care gets undermined, recruiting and retention are more difficult, medical errors can go up because of burnout and patient satisfaction can go down because of staff burnout.
There are human reasons to be attentive to burnout but also financial downfalls if you don't care for colleagues. It translates to the bottom line. It is costly to recruit new colleagues, especially when it comes to physicians and nurses. And when you have to mandate people to work multiple shifts, usual costs become exponentially higher.
So, there are tons of reasons – both human and financial – to pay attention to staff well-being. If you don't it will come back to haunt you and will make your ministry unsustainable.
Read more profiles in the Rising to the Call series.