By LISA EISENHAUER
For Nikki Love-McIntyre, the prospect of dialysis was more intimidating than the prospect of undergoing an organ transplant. "I think that's one thing that just scared the bejesus out of me," Love-McIntyre says of being tethered to a blood filtration machine for hours at a time.

The kidney and pancreas transplant Nikki Love-McIntyre got in October 2015 at SSM Health Saint Louis University Hospital restored her health and made her an advocate for organ donation. She's hopeful that a new federal kidney care initiative will aid others with kidney disease.
Courtesy Mid-America Transplant
Fortunately for her, a suitable kidney was found before the renal disease she had been diagnosed with a year earlier progressed to where she had to have dialysis. But just barely. She was a week away from her scheduled appointment for a fistula.
Love-McIntyre, of Belleville, Ill., underwent a successful kidney and pancreas transplant at SSM Health Saint Louis University Hospital in October 2015. She says her new organs put an end to the misery of renal disease and the diabetes that triggered it.
Now she is hopeful that an executive order signed by President Donald Trump on July 10 will spare others from having to suffer with kidney disease and that, if they do, it will mean more of them will be able to get a life-changing transplant like she did.
"It's going to give more people who are on the waiting list access to organs faster," she says. "I think that's awesome, because I think a lot of people don't understand what someone who is waiting for basically a lifesaving organ goes through."

Lentine
Dr. Holly Kramer, a nephrologist at Loyola University Medical Center in the Chicago suburb of Maywood, Ill., sees much to applaud in the executive order. In fact, she sees it as "the most exciting thing that's happened in the world of nephrology in the past 30 years." The medical center is part of the Trinity Health system.
"It's very comprehensive," says Kramer, who is also president of the National Kidney Foundation. "It's really trying to look at the whole spectrum of kidney disease and trying to incentivize better treatments for those patients and to increase organ transplantation and in-home dialysis therapies."
Specifically, the executive order calls on the U.S. Department of Health and Human Services to:
- Launch a public awareness campaign to increase knowledge of chronic kidney disease. The agency says four out of 10 people with chronic kidney disease don't know they have it.
- Reform the nation's organ procurement and management system to increase the supply of transplantable kidneys.
- Expand support for living donors through compensation for related expenses like lost wages and child care.
- Encourage development of wearable or implantable artificial kidneys, through cooperation between developers and the Food and Drug Administration and support for KidneyX, a public-private partnership between HHS and the American Society of Nephrology.
Like Love-McIntyre, Dr. Krista Lentine applauds the executive order. Lentine is medical director of living kidney donation at the SSM Health Transplant Center at SSM Health Saint Louis University Hospital.
She sees the initiative as recognition of "the need to transform the way kidney care is delivered in this country."
Lentine cites statistics to make her point:
- Of the more than 40 million Americans with kidney disease, 700,000 have end-stage kidney failure that requires dialysis and/or transplant.
- Medicare pays about $115 billion annually caring for patients with chronic kidney disease. The cost to care for a dialysis patient is about $93,000 per year versus $36,000 per year to care for a patient with a functional transplant, after the cost of the transplant surgery.
- The average five-year survival rate after a living donor transplant is about 85 percent and about 75 percent after a deceased donor transplant but only about 45 percent for patients on dialysis.
"We have a situation now where the therapy with the poorest outcomes, on average, is also the most commonly used and the most expensive," Lentine says.
Prospects for better outcomes
Among the aspects of Trump's order that she especially welcomes are its efforts to bring more dialysis services into patients' homes and to move patients off dialysis entirely by giving them kidney transplants.
The advantages to moving dialysis treatment to the home include restoring patients' independence and reducing the cost of treatment.
The benefits of transplantation versus dialysis are more transformative, Lentine says. That is, studies show that untethering patients from dialysis not only improves quality of life but also gives them a longer life span.
Of course, the key to giving more patients transplants is finding more donors. HHS says that as of Jan. 1, there were 100,791 Americans waiting for kidney transplants. According to the National Kidney Foundation, in 2018, 21,167 kidney transplants took place nationwide. Of these, 14,725 kidneys came from deceased donors and 6,442 from living donors. In general, the median wait time for first kidney transplant is three to five years, a number that varies depending on health, compatibility and availability of organs.
Financial assistance
The president's order targets the organ shortfall in several ways. One is to make it less onerous for more people to become living donors by helping to cover related expenses, such as the previously mentioned lost wages and child care costs.

Talone
Sr. Patricia Talone, RSM, views that assistance as potentially particularly helpful for African Americans, a segment of the population that is especially hard-hit by kidney disease and by lower incomes.
The National Kidney Foundation says African Americans constitute more than 35 percent of all patients in the U.S. on dialysis for kidney failure, about three times their representation in the overall U.S. population.
"I am very much against paying for organs, but I think we can ease financial challenges for living organ donors," says Sr. Talone, retired vice president for mission services for CHA and board member emeritus of Mid-America Transplant, an organ procurement organization.
Organ procurement revisions
Another way the executive order aims to ease the donation shortfall is to revise the rules on federally designated organ procurement organizations so that more "transparent, reliable, and enforceable objective metrics" are used by HHS to evaluate their performance.
While the specific revisions of rules for organizations like hers are still being written by HHS, Diane Brockmeier, president and chief executive of Mid-America Transplant, is hopeful that the result is more donated kidneys and fewer rejections of them by hospitals and transplant centers.

Brockmeier
Brockmeier says the number of kidney donations has been on the upswing for eight years, but that increase is dwarfed by the increase in need for kidney transplants.
Brockmeier would like to see HHS revise regulations to encourage hospitals to take so-called high-risk kidneys, including organs from older donors that could be lifesaving for older recipients and organs from HIV-positive patients for transplant into HIV-positive recipients.
Loyola's Kramer says revisions to rules for organ procurement organizations, such as on how they go about contacting treatment centers when they have transplantable organs and when and how biopsies must be done to detect diseases or injuries to organs, could increase the organizations' efficiency.
Vigor restored
Love-McIntyre is doing what she can to get the word out about kidney disease and the need for more organ donors. In the four years since her kidney and pancreas transplant, she has accepted many invitations to speak at events where she tells people how the surgery ended her insulin dependency and restored the vigor that kidney disease had stolen.
"I'm blessed to be here," she says. "I'm blessed to have the opportunity to tell my story."
Kidney Foundation's leader cheers HHS' bold kidney care goals
Dr. Holly Kramer was in the audience at the Ronald Reagan Building and International Trade Center in Washington, D.C., when President Donald Trump signed an executive order in July establishing a bold timetable for improving care of U.S. patients with kidney disease.

Kramer
Based on the order, the Department of Health and Human Services laid out several goals, including, by 2025, having 80 percent of new end-stage renal disease patients either receiving dialysis at home or receiving a transplant. Right now, only about 12 percent of dialysis patients undergo the treatment at home and more than 100,000 people are awaiting kidney transplants.
"Whether or not they're going to be able to make the big goal … remains to be seen, but I think setting a really big goal like that brings a lot attention and energy to the problem," Kramer says.
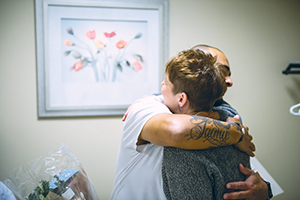
Anthony Gonzalez hugs Lynne Snyder, who had anonymously donated a kidney to him, at the pair's first meeting last month. The successful transplant took place at Loyola University Medical Center in Chicago. Gonzalez's wife was not a match for her husband, but she donated a kidney for someone else on the waiting list.
Courtesy Mid-America Transplant
Kramer is a nephrologist at the Loyola University Medical Center, a Trinity Health facility in the Chicago suburb of Maywood, Ill., and president of the National Kidney Foundation.
HHS also set a deadline of 2030 for doubling the number of organs available for transplant and reducing the number of Americans developing end-stage renal disease by 25 percent.
To get the kidney disease prevention and shift in care of kidney disease that federal officials envision will require hiring more nurses and educators for tasks like teaching patients how to prevent or address kidney disease through diet or how to do their own dialysis treatments in their homes, she says.
"This is a great thing for patients," Kramer says. "I think the doctors are concerned about how are we going to achieve this because the Department of Health and Human Services and Medicare, they're not saying OK here's $40,000 for your dialysis unit to figure out how to increase transplantation education."
Kramer points out that Medicare picks up the cost of caring for patients with kidney failure and that bill is hefty. Care for the 726,000 people in the U.S. with end-stage kidney disease alone accounted for roughly 7 percent of Medicare claims, or $35 billion in 2016, according to federal statistics. (An additional 12.5 percent of Medicare claims, or $79 billion, was paid for treatment of chronic kidney disease that same year.) Meanwhile, the number of people with end-stage renal disease is increasing in the U.S. by 5 percent each year.
Figures like that are alarming, Kramer says, but so is the lack of advancements in kidney care. She is hopeful that the executive order will be accompanied by more investment from the federal government in technologies that improve care, such as better dialysis systems, and more funds for disease prevention programs, especially dietary counseling.
Everything in the executive order, which includes calls for more prevention efforts, more transplants and the development of artificial kidneys, is not only welcome but overdue, in Kramer's view.
"The nephrology community wants to move forward," she says. "We're tired of working in a dialysis unit that looks the exact same as 1982 and we're tired of transplantation and organ procurement that looks pretty much the same as for the past several decades. We want change. We want to make things better for our patients and we want better prevention."
— LISA EISENHAUER