Surgeon practicing at SSM Health academic medical center is developing applications for the technology
By COLLEEN SCHRAPPEN
When Andrew Oberle was brought in to SSM Health Saint Louis University Hospital in 2012, he had suffered almost unimaginable trauma. While working at a chimpanzee sanctuary in South Africa, Oberle, then 26, was attacked by two male chimps. He was torn virtually limb from limb, losing most of his fingers, his nose and both of his ears, and large portions of his scalp, feet, arms, legs and buttocks.

Dr. Bruce Kraemer, left, performed multiple reconstructive plastic surgeries on Andrew Oberle, as he recovered from wounds inflicted during an animal attack. Oberle, at right, now helps other trauma patients build resilience, which he says is essential to recovery.
His initial treatment was at a small hospital in Mbombela, formerly Nelspruit, South Africa. He was moved to a higher acuity hospital in Johannesburg where, about three weeks after the attack, he was revived from a medically induced coma.
After two months in South African hospitals, Oberle was brought home to St. Louis, to be treated at SLU Hospital under the care of plastic surgeon Bruce Kraemer. Kraemer, a professor of surgery at Saint Louis University, practices with SLUCare, the faculty medical practice that staffs the quaternary care academic medical center. Kraemer told Oberle about the plan for his treatment, which included the use of extracellular matrix (ECM) technology.
"He came into my room and told me how he treats wounds," recalled Oberle, now 32. "I was so grateful that someone wanted to take care of me. Even though I didn't understand (ECM), the first time I met him, I trusted him completely."
ECM devices, derived from pigs' bladders, contain no cells, so there is no chance of rejection. Instead, the porcine tissue, comprising proteins, collagen and other biological materials, forms a structural scaffold that supports the patient's own cell growth.
ECM treatment can be used on patients with many different types of injuries: burns, chronic wounds such as ulcers, severe lesions or trauma to the skin, muscles and tendons, and damage to appendages such as fingertips.
The product cannot be used to treat wounds that already have closed, but even two months after the chimp attack, many of Oberle's injuries still had not healed. Kraemer's plan involved the use of ECM treatment from the top of Oberle's head to the bottoms of his feet.
"The beauty is in the science of the device," said Kraemer, who has been with SLUCare since 2004. "Cells are costly; this is the stuff around the cells. It can be saved for years."
The company that makes the ECM wound device, ACell, customizes the porcine tissue into sheets of varied sizes and shapes and it also makes a related powder product than can be sprinkled on top of a wound.
Eventually, the body replaces the device with its own tissue, Kraemer said. "It's 'constructive remodeling,' not regeneration. It builds up tissue."
Growth trigger
In Oberle's treatment, ACell sheets were used on top of his scalp and forehead, which had been ripped open by the chimps. After the forehead tissue healed, it was used along with cartilage from a rib to construct a new nose for Oberle.
A gash on his right cheek was closed up with an almost imperceptible scar that blends in with his skin tone. Kraemer used ACell powder to treat Oberle's left index finger, which had been mostly bitten off. While it does not regrow finger bones, it provides some increased fingertip length.
"At the end of my finger, you can only see a little scar. The incision is not very sensitive," Oberle said, and he can use that finger with his thumb to pinch items. "There's no phantom pain."
Because ECM triggers growth of new, more normal-quality cells, there is less scar tissue and the wound site more closely resembles a patient's healthy skin. This benefit is even more evident in African-American patients, for whom abnormal scarring and irregular pigmentation is more common, Kraemer said.
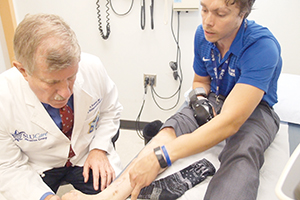
Dr. Bruce Kraemer, a professor of surgery at Saint Louis University, examines his patient Andrew Oberle, who underwent numerous surgical treatments with a biological product that treats wounds by encouraging tissue growth. Kraemer, a plastic surgeon, also reconstructed Oberle's nose following an animal attack.
The healing itself takes longer because the body is replacing its own tissue, but "the overall cost of care is much less. There is less pain and scarring and less swelling," Kraemer said. The device is "a 'basement membrane' that supports skin healing. It's revved up to fight infections and grow skin, so it's a really active layer."
Surgery involving ECM takes less time than the use of skin flaps or transferring tissue from another part of the body. Hospital stays are shorter.
In Oberle's case, most of the initial ECM treatments had healed in about 10 weeks, four of which he spent in SLU Hospital, followed by six weeks at a rehabilitation center. He saw Kraemer about once a week during that time.
"As long as it stays moist and you keep it covered, you really don't have to do much to it," said Oberle, who now works as a development officer and "peer patient advocate" for an institute for trauma survivors named in his honor. The staff of the Oberle Institute at Saint Louis University includes employees of SSM Health Saint Louis University Hospital.
Oberle also credits ECM with saving his right foot after a skin graft done while he was in South Africa started breaking down two years ago. In August of 2016, Oberle had his 26th surgery since the attack, with Kraemer applying ACell sheets and powder to Oberle's foot.
"It's like normal skin," said Oberle, who was able to get back into running after the surgery. "It really lifts my spirits. I'm so happy with how it turned out."
Expanded treatment options
Kraemer has treated about 500 patients with ECM technology since he first used it on a patient with severed fingers in 2010. He is paid consultant for ACell, giving talks about use of the technology to surgeons around the country. As more research has been done over the past decade, he said, the possibilities for ECM use have broadened. Insurance companies are now more likely to cover the treatment, which has U.S. Food and Drug Administration clearance for patients 21 and older.
"The exciting thing is people have options," said Kraemer. "Before, we didn't have options to give them. People are using it more and more around the country, especially in extreme trauma and the orthopedic area."
In the past couple years, ECM use has expanded to include the treatment of cleft palates, scar revisions, hernia repairs and to replace artificial meshes in pelvic surgeries.
Kraemer sees even more potential outside of the United States. In Africa, open cooking in rural villages is a common source of trauma; the porcine bladder powder is simple enough to be applied by a field nurse to treat burns.
"It could change the health care of a whole continent," said Kraemer. "It's got some wonderful applications if you open up to that."
Copyright © 2018 by the Catholic Health Association
of the United States
For reprint permission, contact Betty Crosby or call (314) 253-3490.