By LISA EISENHAUER
When Hurricane Ida was churning across the Gulf of Mexico in late summer, Our Lady of the Lake Regional Medical Center in Baton Rouge, Louisiana, had to brace for a disaster on top of a crisis.
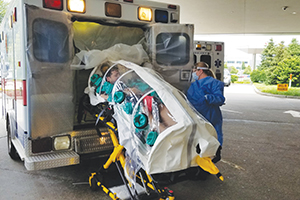
In this disaster drill staged at Mercy Hospital St. Louis before the pandemic, a participant posing as a patient exposed to ebola is enclosed in a portable isolation chamber for transport.
The medical center was in the middle of its worst surge in COVID-19 cases since the start of the pandemic. The patient load was so heavy that the hospital had halted elective surgeries and a team of military doctors and nurses was assisting its staff.
Ida roared ashore just before Labor Day, causing 26 deaths in Louisiana and wreaking billions of dollars in havoc across its multistate path. At Our Lady of the Lake, damage was minimal and its patients and staffers unharmed, an outcome that Jeff Mosely, one of the disaster preparedness planners for the hospital and its related facilities, credited to a combination of long-term planning and incident-specific flexibility.

Mosely
Emergency managers at some other Catholic health systems that have faced emergencies amid the lingering crisis of the pandemic say similar strategizing and agility have seen their systems safely through.
Decisions pay off
Mosely can cite several examples of decisions that enabled Our Lady of the Lake to stay open and minimize COVID-related risks during Ida:
- As the storm hit, Our Lady of the Lake switched to the generator system fueled by natural gas it had invested in after an outage caused by Hurricane Gustav put the medical center on the brink of calamity in 2008. If not for the generators, the medical center would have lost power like much of Baton Rouge.
- The roofs of many of Our Lady of the Lake's structures had been upgraded and storm-hardened in the last five years as part of a $4 million upgrade program. Only one structure, a medical office building, lost its roof membrane during Ida.
- Temporary sleeping areas for staff were spread out across more spaces in the hospital and with smaller groups in each to allow social distancing during the pandemic. As an added safeguard, Mosely bought about 100 one-person pop-up tents so staffers in the largest groups would have some personal space.
- With gas stations closed because of ongoing power outages, Mosely arranged to have gasoline brought in by tankers. The hospital distributed free fuel to staff for about four days.
Like all other accredited hospitals, Our Lady of the Lake is subject to the Joint Commission's requirements to activate or simulate the activation of an incident command to handle a disaster at least twice a year.

A worker at Our Lady of the Lake Regional Medical Center in Baton Rouge, Louisiana, pushes his car after running out of gas while waiting in line for a free fill-up. The hospital brought in the gasoline tanker in late August to help its workers after Hurricane Ida caused power outages that forced gas stations to close.
In Mosely's six-year tenure as the medical center's vice president of construction and facilities, mock disaster drills have been unnecessary. "Since I've been in Louisiana, we haven't had to do a simulated event because we've had more than two real ones a year," he says. (In October, Mosely became system vice president for construction for Franciscan Missionaries of Our Lady Health System, Our Lady of the Lake's parent system.)
Prepping and stockpiling
Jake Parmentier, emergency manager for Chesterfield, Missouri-based Mercy, says pandemic-related infection precautions have prompted Mercy to take some of the drama out of emergency disaster drills conducted at its hospitals. There have been no mock victims from schools or community agencies it partners with in emergency planning.

Parmentier
Parmentier says one of the disaster scenarios that figures prominently into Mercy's emergency planning is tornadoes, a high risk for the Midwestern system. Mercy continues to follow practices adopted after an F-5 twister made a direct hit on its hospital in Joplin, Missouri, in 2011. One is to keep a stash of "go bags" with the basics including water bottles, a flashlight and pens so
co-workers could document things including care interventions or where they moved a patient to get them out of harm's way.
The Joplin tornado also made clear the need for backup communications capabilities. That prompted Mercy to partner with the Missouri Hospital Association to build a mobile emergency communications facility that can establish Internet, phone and two-way radio access in a disaster.

A sign posted on a door at Mercy Hospital St. Louis alerts staff and visitors that a disaster drill is underway.
"Essentially, we're able to stand up an entire communications department inside of a trailer," Parmentier says. Mercy is in the process of adding a second mobile facility that could be dispatched to a disaster area anywhere in the system's catchment area, which, in addition to Missouri, includes the tornado alley states of Arkansas, Oklahoma and Kansas.
In February, Mercy put its emergency processes in place when a fire forced the brief closure of its hospital in Cassville, Missouri. Parmentier says the system's long-term preparation and training clicked and it adhered to pandemic modifications: All patients and staff safely evacuated from the hospital, and transporters and admitters followed COVID protocols as patients' care was shifted to a nearby Mercy hospital and no subsequent safety issues arose.
"You never want to have to exercise your emergency preparedness plans in true fashion, but when you do it's nice to be able to see that they work, that all of your training and education didn't go to waste and you're actually able to complete the task at hand," he says.
Northwest heats up
Grant Finch, emergency management coordinator for the PeaceHealth Oregon network, says the effectiveness and flexibility of his system's disaster protocols have been put to the test on several occasions during the pandemic.

Finch
In late summer 2020, PeaceHealth went into emergency operations mode as wildfires spread close enough that dense smoke could be seen from some facilities. At the time, the region's acute care resources were maxed out by COVID. "We were already full at the hospitals as a state," Finch recalls.
He and other PeaceHealth emergency planners stayed in close contact with fire chiefs and emergency management officials and identified potential backup care sites. In the end, the fires never got so close that PeaceHealth had to close facilities or evacuate patients.

A crew with McKenzie Fire & Rescue Fire District gathers at the scene of a wildfire that came within a few miles of PeaceHealth Sacred Heart Medical Center at RiverBend in Springfield, Oregon, in September 2020. Charene Dehne, a nurse manager at PeaceHealth's hospital in nearby Eugene, Oregon, captured this image. Dehne volunteers with the crew as an emergency medical technician.
The system assisted with housing for some of its care providers whose homes were either destroyed or threatened by the fires.
This summer, when temperatures in the temperate Northwest reached all-time record highs, PeaceHealth prepared to activate its plan in the event excessive heat spiked demand so much that it knocked out power to those in hospice or home care settings. The plan includes working with emergency response partners to provide generators and transport patients to alternative care sites.
"A lot of our patients on that service line are dependent on power, they have medical equipment, they need oxygen, but they are in their homes," Finch says.
The heat wave, while causing misery for many, didn't spiral to the level that it required PeaceHealth to go into disaster response mode, Finch says.
Emerging threats
He and disaster planners at the other systems say because of the heightened threats posed by global warming, weather emergencies like heat waves, fires and tornadoes are figuring more and more prominently into emergency planning. And they are not the only emerging threats. With modern health care highly dependent on technology, cyber failures and ransomware attacks also have moved to the top of the sector's list of vulnerabilities. Another threat that has rocketed to the top is pandemics, spurred by COVID's unexpected emergence and tragic toll.
The evolving risks compound the challenges for disaster planners.
"When you start stacking incidents and stacking emergencies on top of one another, they do start to interfere with one another and it becomes a more complicated situation," Finch says. "You do have to be flexible in your planning and in your response because what you thought might happen and the way you thought you might get out of it isn't going to work."