By LISA EISENHAUER
Providence St. Joseph Health, Ascension and Trinity Health, the three Catholic health systems that were among the first to test the concepts behind an initiative to make care for older adults more age-friendly, have since made the framework their own by adding local adaptations.

Dr. Cara Ellis discusses fall risk factors with Larry, a volunteer older adult patient, as part of the geriatric mini fellowship at Providence St. Joseph Health in 2018.
Photo courtesy of Providence St. Joseph Health
The framework that is at the core of the Age-Friendly Health Systems initiative is called the "4Ms" for what matters to the patient, mentation, mobility and medication. (See Page 2 sidebar.) Providence Oregon put it in practice in outpatient care at the regional system, part of Providence St. Joseph Health, in 2017.
The idea, says Colleen M. Casey, associate clinical director of Providence Oregon's Senior Health Program, was to "train up the workforce" because there simply weren't enough people trained in geriatric care. Based on census data, projections are that by 2034, there will be more people 65 or older than people 18 and younger for the first time in U.S. history. Meanwhile, the number of geriatric-trained clinicians is expected to grow at a much slower pace than that of the senior population.

Casey
"We identified that if we could bring both the skills that would be needed and the framework of the 4Ms to operating frontline clinical care teams, that would be a way to augment the work of the small few of us," Casey says.
Go big
Last year, Providence St. Joseph Health decided to adopt the age-friendly framework for all patients.
Leslie Pelton, senior director at the Institute for Healthcare Improvement and leader of the Age-Friendly Health Systems initiative, says there is worldwide interest in the framework. "I find out literally every day there's adoption of the 4Ms in places I don't know about, which is terrific."

Pelton
Pelton has been contacted by health systems in Australia, India and Scotland about how to put the 4Ms in place. "Our aim was to ensure that evidence-based care was practiced everywhere that older adults showed up," Pelton says. "I think 4Ms as an organizing framework is just the right level of complexity, if you will. It's very accessible."
The 4Ms, Pelton says, "are a framework, not a model, not a program, which means we very intentionally left lots of space for local adaptation because the research and IHI's experience is that if you leave a lot of room for local adaptation, people are more likely to pick this up and make it their own and the change and improvement will be more sustainable."
Helping avert crisis
Providence Oregon used the framework when it standardized the protocols for screening and intervention for fall risk among its 80,000 patients who are 65 and older who are cared for in its primary care practices. Falls are a leading cause of death and disability in older adults. With standardization, the screenings grew from 17,000 patients seen in its clinics in 2016 to 35,000 in 2019.

Dr. Melissa Calhoun and Dr. Eric Webb practice a fall risk assessment with Rachel, a volunteer older adult patient, during a session of the Providence St. Joseph Health geriatric mini fellowship in 2019. Falls hamper mobility and are one of the major causes of fatal and nonfatal injuries for people age 65 and over. Keeping older patients mobile is one of the focuses of the Age-Friendly Health Systems initiative.
Photo courtesy of Providence St. Joseph Health
To expand the use of the age-friendly framework, Casey and her colleague Dr. Marian Hodges, a specialist in geriatric and internal medicine, founded a geriatric mini fellowship. Its four-week curriculum unfolds in one-week increments over the course of a year. Six or seven physicians or nurse practitioners can take part each year. By the end of 2019, 11 graduates of the mini fellowship had together given 50 presentations to colleagues, developed workflows for geriatric care in their clinics, led geriatric improvement projects and provided consultations for complex geriatric cases.
"The idea is that we're not only training them to change their practice but we're steeping them in the ingredients of systems change so they become their own change agent, with our help, and become the geriatrics experts by default in their own clinics to continue the ripple effect of change," Casey says.
Systemwide adoption
Last year, the clinical leadership of Providence St. Joseph Health voted to adopt the age-friendly framework not only systemwide but for all patients, while keeping the priority on those 65 and older. They also added a fifth "M" for malnutrition. The decision came after what Deborah Burton, senior vice president and chief nursing officer, says was a formal debate over whether the initiative was appropriate and scalable for such a big system.

Burton
The bundle of practices that the system created under the initiative was set to go in place early this year. However, the plans were delayed when the coronavirus pandemic hit. The initiative began to roll out across the system in late summer, starting in acute care facilities but with plans to bring it into use at all sites and by all providers within months. This fall the system is building a dashboard to monitor related metrics, such as whether goals of care and advanced directives are being discussed with older patients.
"It's like motherhood and apple pie," Burton says of the framework. "Who can argue with doing the right thing for the elderly in an evidence-based, and I don't want to say simple, but certainly straightforward way?"

Staschke
Denise Staschke, director of post-acute and senior services within Ascension St. Vincent Medical Group in Indianapolis, says nurses doing Medicare wellness assessments use the 4Ms framework to get a baseline, so that when things do start to change for an elderly patient, the nurses are readily able to pick up on that.
Ascension St. Vincent also started a geriatrics mini fellowship. Primary care clinics can send their entire staffs for six one-hour sessions that dive into the 4Ms training. Staschke says of the age-friendly training: "We all want this to continue."
The framework has worked so well in the outpatient setting that Ascension St. Vincent started an inpatient geriatric consultation program called Mobile ACE (Acute Care for the Elderly) that is making use of the framework. Under the program, a team with a nurse practitioner and a nurse get referrals from other providers for older patients suffering from or at risk of problems such as delirium and come up with care plans.
The invisible patient
Carrie Hays McElroy is chief clinical and compliance officer for Trinity Health PACE, a group of 10 Programs of All-Inclusive Care for the Elderly. Because these programs already incorporated much of the 4Ms framework, McElroy was involved with crafting the pioneer work within the health system around the initiative. The ability to expand across other Trinity Health ministries has been limited recently, she says, but she is seeing an upswing now, including a push to have it championed by the system's population health leaders who would share it among the physician practices affiliated with Trinity Health.

McElroy
"We're really hoping this is practiced across the continuum, it's not just in the emergency departments, it's not just acute care, not just in the nursing home setting, that it's also in the physician offices," McElroy says.
Lisa Zapatka, Trinity Health Of New England's chief nursing officer, oversees a pilot of the age-friendly initiative at Johnson Memorial Hospital in Stafford Springs, Connecticut. When a patient who's 65 years or older is admitted, caregivers do assessments for mobility, medication and delirium. The care providers also have a conversation with the patient about what matters to him or her.
"The goals of care are then geared toward what that patient really wants, and we want that conversation to happen on almost every encounter," Zapatka says. "Sometimes older adults feel invisible. We want them to be visible. We want them to be heard. We want them to know we're listening to them."

Zapatka
She hopes the pilot project ends up being replicated at all Trinity Health sites across her region. "It's not fancy, high-tech work but it can really be a foundation of what can keep our patients safer when they do have to come into our hospitals and if that's continued along the continuum, then it's just good care for the patient," she says.
Zapatka thinks the 4Ms should be a topic of conversation with patients just as other aspects of care are.
"What I would love to see, once we have this more hardwired, is that we discuss this with the patient, because quite honestly this initiative really aligns with our beliefs at Trinity Health and I think with other Catholic health systems," she says. "That is, we respect the individual and in doing that we personalize their care, we are partners in their care and our basic promise is to keep them safe. Age-friendly care helps do that."
'4Ms' frame age-friendly care
The Age-Friendly Health Systems initiative is based on a simple set of practices called the "4Ms" — what matters to the patient, mobility, mentation and medication.
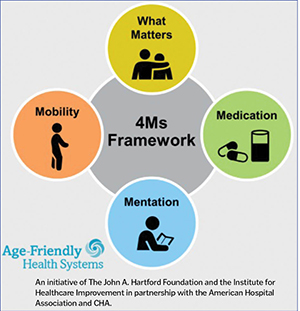 The initiative was started by the Institute for Healthcare Improvement, a nonprofit focused on motivating and building the will for change, and The John A. Hartford Foundation, a private philanthropy whose goal is to improve the health of older Americans. CHA and the American Hospital Association are partners on the initiative that have worked to promote and expand it.
The initiative was started by the Institute for Healthcare Improvement, a nonprofit focused on motivating and building the will for change, and The John A. Hartford Foundation, a private philanthropy whose goal is to improve the health of older Americans. CHA and the American Hospital Association are partners on the initiative that have worked to promote and expand it.
Julie Trocchio, CHA's senior director of community benefit and continuing care, says she joined the age-friendly bandwagon early on because she saw its framework as "just basic good care for older people" that is built on evidence-based practices. "I would say the goal was to close the gap between what we know how to do, what the research tells us and what we actually do," Trocchio says.
Leslie Pelton, senior director at the Institute for Healthcare Improvement and leader of the Age-Friendly Health Systems initiative, says it was with that prospect in mind that IHI and the Hartford foundation brought thought leaders in geriatrics together to analyze existing geriatric care models, consolidate evidence and lessons learned, and collaborate with other health care experts. The result was the 4Ms, described like this:
• What matters — Know and align care with each older adult's specific health outcome goals and care preferences including, but not limited to, end-of-life care, and across settings of care.
• Mentation — Prevent, identify, treat and manage delirium across settings of care.
• Mobility — Ensure that each older adult moves safely every day to maintain function and do what matters.
• Medication — If medication is necessary, use age-friendly medication that does not interfere with what matters to the older adult, mobility or mentation.
There are three on-ramps that systems can take to join the initiative. Systems can become part of an "action community" that tests the 4Ms framework in hospital and ambulatory settings and shares learnings in a seven-month program; systems instituting the framework can bring IHI in as a consultant; or systems can institute the age-friendly practices on their own initiative and share their approach with IHI.
Once hospitals or practices incorporate the 4Ms into patient care, IHI provides them with a toolkit to market themselves as an Age-Friendly Health System.
— LISA EISENHAUER
Trials of pandemic underscore importance of spelling out care wishes before crisis strikes
The challenges and turmoil brought on by the coronavirus pandemic have reinforced the importance and validity of the Age-Friendly Health Systems, say some care providers.

Moccia
Michelle Moccia, director of the geriatric emergency room at St. Mary Mercy Livonia in Michigan, recalls that early in the crisis she and her colleagues cared for many critically ill elderly patients who could not articulate their care preferences and did not have an advanced care plan or individual with medical power of attorney identified in their medical record. The hospital is part of the Saint Joseph Mercy Health System, a subsidiary of Trinity Health.
"Unfortunately, many older adults arrived in our emergency center with COVID-19 and we really didn't have an understanding of what matters to them. Did they want to be put on a ventilator? What did they want their end-of-life care to be? Did they have a surrogate who could help make decisions for them?" Moccia says.
If they couldn't reach families or if the families were unaware of the patients' wishes, the care providers in the ER followed still-evolving best medical practices, including at times using extraordinary interventions such as intubation to keep the patients breathing. "That was very distressful for many of us," she says of ER workers who had to make major treatment decisions on their elderly patients' behalf.
In recent months, care protocols have gotten more standardized with intubations used as a last resort. Meanwhile, Moccia has come to see the earlier frenzy as validation of the foundations of the age-friendly framework, especially the "what matters" aspect of care. "It really brought it to the head that it's very important as we grow older that we have these discussions with our family members about our end-of-life care and choosing someone to speak for you in case you can't speak for yourself," she says.
Knowing what matters
Deborah Burton, senior vice president and chief nursing officer at Providence St. Joseph Health, says that early in the pandemic it was apparent that the elderly were at heightened risk of dying from COVID. "The focus was on getting the older patients the care that would save them, including intubating them early if they were at high risk for stopping breathing in the intensive care unit," Burton says.
Sometimes that care came without conversations with those patients about whether they wanted to be intubated, sent to the ICU or even admitted to the hospital rather than being cared for at home, she says. The way to avoid that in the future is to have goals of care conversations with every patient before there's an emergency, Burton says.

Moore
Andria Moore, nursing practice and quality program manager for Providence St. Joseph Health, says just as COVID was beginning to take its tragic toll, Providence St. Joseph Health was starting to roll out the framework for use systemwide. Because of COVID, the system put that plan on hold until this fall. The principles of the framework nevertheless were already gaining wide acceptance among care providers.
"We realized that the pandemic both reinforced and accelerated our commitment to becoming an Age-Friendly Health System," Moore said during a webinar in September on the age-friendly initiative. The webinar was sponsored by Modern Healthcare and The John A. Hartford Foundation, the philanthropy that has funded the initiative.
Toll on care providers
Moore says as a result of the isolation and drop in support services due to the pandemic, caregivers noticed an accelerated decline in many older patients, such as decreases in mobility along with an increase in falls, more incidences of delirium and a worsening in their overall mentation. Those issues along with monitoring medication and knowing what matters to patients are among the main focuses of the age-friendly initiative and its goal of giving older patients the healthiest and most satisfying life possible.
The demands of the pandemic exacerbated by the prohibition on visits by loved ones of terminally ill patients also took a toll on clinicians, Moore says. "They were demonstrating signs and symptoms of moral distress not only related to COVID and everything that that brought onto them, but also about whether they were able to meet our patients' true needs and having to function not only as the role of the nurse but as the family members, the hospice provider, etcetera," Moore says.
She says the pandemic highlighted for those clinicians the value of the foundational elements of age-friendly care, especially the importance of identifying and keeping sacred what matters to patients. It also brought to the fore new challenges, such as how to honor patients' wishes when their condition is worsening rapidly, and no advocate is at their side.
The pandemic's lessons are being incorporated into the trainings and discussions Providence St. Joseph Health is using as it puts the age-friendly initiative into wider practice.
Moore and Burton say another lesson from the pandemic is how useful telehealth can be, especially for those who don't want to leave their homes or congregate living centers during the pandemic. "We learned to use telehealth and to do things we had never really done before with keeping people well supported, cared for and safe in their homes," Burton says.
As painful as the pandemic has been, Burton says it has brought Providence St. Joseph Health together in many ways, including sharing the evidence-based practices of the age-friendly initiative and breaking through silos to work across the care continuum to improve patients' outcomes. "We are a stronger, more unified, more patient-centric organization because of COVID. I wouldn't want to relive COVID to get there again but it is a certain gift we got from COVID."