By JULIE MINDA
By the time husband and wife William and Teri Welder sought dental care at the Mount St. Mary's Neighborhood Health Center in Niagara Falls, N.Y., last year, both had suffered for more than a decade with dental pain and decay.
"I only had two teeth left — they were on the bottom — and I couldn't hardly eat, I refrained from going out, I didn't want to eat in public or smile," said Teri Welder, 55. Both she and her husband, age 61, had quit going to the dentist around 2002 after they both lost their jobs because of poor health. They qualified for Social Security disability benefits and Medicare, but the money doesn't go far and Medicare doesn't pay for fillings, extractions or dentures.
During William Welder's decade-plus without dental care, nearly all his teeth decayed. "I couldn't afford a dentist, so I pulled three or four of my own teeth," he said. Most of the rest fell out.
The couple learned about Mount St. Mary's oral health program for the uninsured and underinsured during one of William Welder's medical visits to the neighborhood health center.
Over the course of about a month and a half, both Welders had their remaining teeth pulled at the center, Teri received antibiotics and pain medications, and then both were fitted for the dentures they started wearing about 10 months ago.
"I'm smiling more now, and I'm happy to take pictures with my great-grandkids," said Teri Welder.
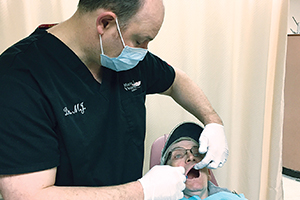
Dr. Mario J. Violante III, treats patient Raymond Jasper at the Mount St. Mary's Hospital Neighborhood Health Center in Niagara Falls, N.Y.
Mount St. Mary's Hospital and Health Center in Lewiston, N.Y., part of Catholic Health System of Buffalo, N.Y., is among many ministry providers that have invested in dental services for low-income people who are uninsured, underinsured and Medicaid-insured. Representatives of dental centers run or supported by ministry providers said their organizations are motivated by a desire to ensure all community members get dental care, regularly and in the appropriate venue — and to reduce the use of the emergency department for oral health care.
Right location
Ministry providers that have made dental health a priority include Mount St. Mary's, with its support of a partner-run dental clinic colocated with a family health clinic; Mercy Health — Youngstown, Ohio, with its clinic housed in an ambulatory care center at its Youngstown hospital; and Providence Milwaukie Hospital in Milwaukie, Ore., with its partner-run clinic housed on the hospital campus.
These ministry dental services rely on partnerships. Providence Milwaukie has a federally qualified health center as a partner. Others partner with community service agencies, funding organizations or dentistry schools. All seek to provide a dental home for their patients, so that the patients will get routine, preventive care to avoid dental crises. All receive referrals from the Catholic hospital hosting or supporting them.
Dr. Jane Grover, director of the Council on Access, Prevention and Interprofessional Relations for the American Dental Association, said to her knowledge no one has compiled a count of hospitals with dental clinics. Yet, such services in recent years are "higher on the radar" of hospitals, partly because oral health has a direct influence on a person's overall health status.
Dental care also is a concern for hospitals because the use of the emergency department for dental care has been increasing nationally. A study by the American Dental Association found that emergency department visits for dental reasons rose from 1.1 million in 2000 to 2.1 million in 2010.
Domino effect

Beck

Franjoine

Jones
Dr. Jonathan Hall is dental director of the Neighborhood Community Health Center, the FQHC-operated dental clinic at Providence Milwaukie. He said if people neglect their oral health, they may end up in the emergency department with severe tooth pain, infection, swelling or abscesses.
Only rarely can the emergency department treat the true source of the pain, be it a decaying or fractured tooth, damaged root or other dental condition, said Dr. M. Frank Beck, director for a general practice dental residency program at Mercy Health. He said emergency departments typically address the symptoms of dental pain by prescribing antibiotics and pain pills. The Youngstown hospital's protocol is to refer emergency department patients with dental issues to the clinic for care that solves the underlying dental problems.
Left untreated, Beck said, "Dental problems don't get better, they get worse. And your third time back to the emergency department, you may need inpatient care or two or three days of services."
An analysis of data from the Healthcare Cost and Utilization Project identified abscesses, cavities, periodontitis, gingival disorders and disorders of tooth development and eruption as the top five dental conditions that resulted in inpatient admission from the emergency department. The utilization project is a comprehensive source of hospital data sponsored by the Agency for Healthcare Research and Quality.
Beyond such dental crises, unaddressed oral health issues can exacerbate chronic conditions, which also can lead to hospital admissions, said Bernadette Franjoine, vice president of mission integration for Mount St. Mary's Hospital and Health Center. Beck of Mercy Health concurred, saying evidence shows that oral inflammation can contribute to other serious conditions, including heart disease, hypertension and sleep apnea.
Beck said that contaminated dentures can spread pathogens that can cause pneumonia. Poorly controlled periodontal disease in a diabetic patient can result in increased bacteria in the blood, inflammation and corresponding immune responses that increase insulin resistance, Beck said. Conversely, improving oral health significantly improves blood sugar stability.
Gateway to the body
Franjoine said that because of the interconnection of dental and medical health, "clinical providers have long recognized the need to integrate oral health into the overall assessment and management of patient populations," but it historically has been difficult to make a case for hospitals operating dental clinics. She said now that facilities increasingly are building partnerships to address population health concerns, it is becoming more feasible to build dental care programs.
Hall of the clinic at Providence Milwaukie said, "We're definitely seeing more attention paid to the mouth (by the health care field). We're putting the mouth back in the body, so to speak. We're seeing more attention to integrated care of the patient and treating the whole body."

Teri Welder, top row, and William Welder, bottom row, before and after receiving their dentures at Mount St. Mary's Neighborhood Health Center in Niagara Falls, N.Y.
Dignified care
Most of the ministry providers who spoke to Catholic Health World said their organizations had seen emergency department visits for dental issues drop once patients instead began turning to the appropriate place for such care, the dental clinics.
Beck and Crystal Jones, grant director for Mercy Health —Youngstown, said having dental services available to vulnerable populations can have life-changing implications: Good dental health can improve general health, pave the way for better job prospects and fewer job absences and set the stage for better management of chronic diseases.
Hall said people appreciate getting services from a location that honors their dignity. "They are extremely grateful for the care and attention and the love we're trying to show them. Typically, the patients we're seeing haven't had much attention paid to them. They're used to being written off. But, we try to understand where they're coming from. We listen to them and their story."
| Low-income adults fail to get needed dental care
Low-income adults are failing to get the dental care services they need. An October 2014 research brief from the American Dental Association's Health Policy Institute says that dental care use among low-income adults declined in the vast majority of states between 2000 and 2010, in large part because of poor insurance coverage and poor reimbursement rates in many state Medicaid programs.
According to the institute's brief, states decide whether and to what extent to offer dental benefits to Medicaid-insured adults. The Kaiser Family Foundation says 31 states and the District of Columbia have opted to expand Medicaid eligibility in connection with Affordable Care Act reforms, and 19 states have not. According to a February analysis by the Center for Health Care Strategies, "nearly all states and the District of Columbia offer some dental benefit to their base adult Medicaid population. Thirty-three states cover services beyond defined emergency situations. … Among those, 15 offer extensive services." That analysis said 29 of the 31 states currently expanding Medicaid are offering or plan to offer the same dental benefits package to both their base and expansion populations. Tavia Hatfield is regional director of community services for Covenant Health of Lubbock, Texas, which operates a dental center and mobile dental unit for low-income uninsured and underinsured people as well as for those insured by Medicaid and the Children's Health Insurance Program. Hatfield said low-income adults have very limited dental coverage in Texas, a state that did not expand Medicaid. She explained that, even for those who do have government-funded insurance, that insurance typically does not cover dental services. She added that the high cost of dental care keeps the uninsured away from the dentist, and high out-of-pocket costs can be prohibitive for working people with high-deductibles on dental coverage plans. People also avoid dentists because of difficulties with getting transportation to appointments, she said. Compounding such concerns is the "tyranny of the moment" that can drive priorities for poor men and women. Crystal Jones, grant director for Mercy Health — Youngstown, Ohio, said, "It's easy to let go of oral health until it becomes a crisis and you're in severe pain. … When you're in poverty, maybe you're trying to get your car fixed, and you're a parent juggling a lot of things. You don't have time for oral health." Dr. Jane Grover, director of the Council on Access, Prevention and Interprofessional Relations for the American Dental Association, added that about half of adults with dental coverage don't use it. "Oral health care is puzzling to people. We don't discuss it as part of our cultural norm. … And, when it comes to the uninsured, many are unaware where care even exists." Dr. Jonathan Hall is dental director of the Neighborhood Community Health Center, a federally qualified health center-operated dental clinic at Providence Milwaukie Hospital in Milwaukie, Ore. He said, "Many people don't come in because there's a lot of anxiety around dental care. They're terrified to come in." Hall said that even when low-income people are willing to come in, and while Oregon's Medicaid program offers relatively rich dental benefits for adults (and that state did expand Medicaid eligibility), "the vast majority of dentists (locally) don't accept Medicaid," in large part because reimbursement rates are low. The Health Policy Institute brief bears out Hall's claim. The brief says in many states there is a shortage of dental providers willing to participate in Medicaid. The brief said this is in part because of "a high rate of cancelled appointments among Medicaid enrollees, low reimbursement rates, low compliance with recommended treatment and cumbersome administrative procedures." Grover of the American Dental Association said provider participation in Medicaid is much better in states that not only offer healthier reimbursement rates but that also have Medicaid policy that is friendly to providers. Such policies remove bureaucracy and administrative headaches so it is simpler to take part, she said. For instance, she said, Maryland recently has enacted reforms that make participation in Medicaid easier for providers, and it saw a resulting increase in providers signing on to serve Medicaid-insured patients. Grover mentioned Arkansas, Nebraska and Oklahoma as other states with high percentages of dentists treating Medicaid patients. |
Copyright © 2016 by the Catholic Health Association
of the United States
For reprint permission, contact Betty Crosby or call (314) 253-3477.