Health care landscape changing quickly; chaplains must adapt
By JULIE MINDA
The sweeping waves of change that have been reshaping health care delivery in the U.S. in recent years also have been fundamentally altering the role of the health care chaplain.
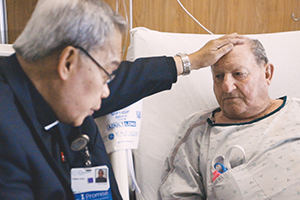
Fr. Eoli Roselada, OFM, a chaplain at HSHS St. Elizabeth's Hospital in O'Fallon, Illinois, blesses Sammie Story. While bedside patient care remains a vital part of chaplaincy, the role has expanded to include much work outside of hospital walls.
Just like their clinician counterparts, health care chaplains have been using metrics in order to quantify their contributions to patient care. They must adhere to standardized protocols, integrate their work with that of clinical colleagues, increase their physical and virtual presence in outpatient care, and respond to expanded expectations for addressing spiritual, emotional and even socioeconomic needs of patients.
To stay ahead of these amplified expectations and ensure patients and others get the spiritual care that is a hallmark of Catholic health care, chaplains must continually learn and adapt.
"We need to be nimble," says Tim Serban, chief mission integration officer for Providence in Oregon, a member of Providence St. Joseph Health.
"We must accept change even if we don't understand it," says Tweeter Henseler. She is manager of chaplaincy at Avera Sacred Heart Hospital in Yankton, South Dakota.

Mercy Chaplain Chuck Russo, at left, takes part in a blessing ceremony at Mercy-GoHealth Urgent Care in Oakville, Missouri, on Sept. 6. Chaplain presence is increasing in outpatient venues.
"We have to be creative," says Joby Brown, staff chaplain at Ascension Columbia St. Mary's Hospital Ozaukee in Mequon, Wisconsin.
"Chaplains have to have the mindset and the heart-set to meet patients and families where they're at — we can't get set in a specific way of doing ministry," says Art Maddock, manager of pastoral services for Mercy Northwest Arkansas. "We have to be flexible."
Credentials and standards
Organizations including CHA, the National Association of Catholic Chaplains and the Association of Professional Chaplains have been contributing to the development of professional standards and educational and training expectations. (See sidebar for a related CHA initiative.)
Requirements and prerequisites to be a chaplain have increased, says Maddock. There is more clarity and definition around what chaplaincy is and the protocols chaplains should follow in delivering their services, says Serban.
Many chaplains are taking continuing education courses to close knowledge gaps, says Sue Kellett, a chaplain at SSM Health Saint Louis University Hospital.

Chaplain Joby Brown, center, meets with intensive care unit associates during a team huddle at Ascension Columbia St. Mary's Hospital Ozaukee in Mequon, Wisconsin. He gets updates on existing patients and learns about newly admitted patients. This helps him to prioritize his work.
Victoria Schmidt
The push toward better defined roles, credentials and standards has included increased research nationally into chaplaincy's impact on patient outcomes, and this research is providing evidence for the value of chaplain encounters, says Serban.
Henseler adds that this quest to show value is happening on a facility level too. She and other chaplains are using metrics to track their activity and aim to tie that activity to patient outcomes.
Team players
Serban says chaplains are demonstrating they can be important patient advocates and help people anticipate the emotional, spiritual and practical struggles they may encounter as they cope with chronic or progressively debilitating illness. Chaplains can help them develop plans to lessen those struggles.
Kellett says as chaplains establish the value of their services, they are earning more responsibility in the patient care process.

Art Maddock, manager of pastoral services for Mercy Northwest Arkansas, blesses the hands of co-workers at Mercy Hospital Northwest Arkansas in Rogers.
Charlie Dey, the chaplain team manager at SSM Health Saint Louis University Hospital, agrees that chaplains are gaining increased acceptance and respect from administrators and clinician colleagues, for what they can add to a patient's experience. Chaplains are participating in interdisciplinary care teams to a greater degree than in the past.
Henseler of Avera Sacred Heart says chaplains' integration into multidisciplinary care teams is reflected in the spiritual care screening questions posed in the medical intake process, so that patients with pressing spiritual needs can be referred to a chaplain. Chaplains also are being included in unit huddles on quality patient care.
Chaplains routinely exchange information with their clinician counterparts through the electronic medical record, and verbally.
Specialization by diagnosis
As systems and facilities are recognizing the value of chaplain care, they are seeking to expand chaplains' presence — especially into areas of service line growth.
Mercy of Northwest Arkansas is part of the Mercy health system of Chesterfield, Missouri. Maddock says because the majority of health care is provided on an outpatient basis, the Mercy system has been active in expanding chaplain services throughout its growing clinic system and into its home care service line.
Saint Louis University Hospital is increasingly embedding chaplains into specialty clinical teams, including neurology, transplant, trauma, triage and the intensive care unit. Dey says the hospital is greatly benefitting from doing so.
Henseler says Avera Sacred Heart is providing dedicated chaplain time in its cancer center, in eldercare facilities and in hospice and palliative care. Brown says Ascension uses chaplains with specialization in such areas as cardiology, oncology, rehabilitation and behavioral health. He says that pastoral education and accrediting agencies offer advanced certifications for such work. Chaplains with advanced training in palliative care and hospice may be helpful to late-stage oncology patients, he says.
Brown notes that the Ascension system is aiming to offer spiritual care in an on-demand capacity in acute and outpatient settings.
Chaplains are increasingly connecting with pa-tients online through telehealth platforms. "Whether we are pulling up a physical or a virtual chair, what we are doing is creating that sacred space to hear the patient," Maddock says.
Chaplains also are increasing their ministry to staff. Maddock says chaplains provide affirmation and an attentive ear. Serban says chaplains offer emotional support as the staff deal with the stresses of delivering care, often to people in trauma. Henseler educates staff on self-care and helps staff tend to their emotional health after painful experiences, such as the death of a patient.
Spiritual triage
With chaplains now taking on expanded responsibilities and increasing their presence throughout the continuum of care and with colleagues, they are pulled in many directions, says Serban. There's a limited number of chaplains to meet increasing demand in a growing number of venues, says Brown.
Maddock says the situation has forced chaplains to prioritize the patients who receive services. Many chaplains used to go room to room in hospitals visiting patients to determine whether an individual was receptive to spiritual counseling. Nowadays, there is little time for those casual conversations. Ministry facilities increasingly rely on screening systems to identify patients in crisis or with serious illness, who may be most in need of chaplaincy services.
At Saint Louis University Hospital, an urban academic medical center with a high-acuity patient population, Kellett says many patients require extensive support for socioeconomic and mental health needs too. She says she and her chaplain colleagues work collaboratively with social services staff to help such patients access the help they need. Dey says this is increasingly important to meeting patients' complex needs.
Ascension's Brown finds the changing demands and responsibilities of the chaplain role exhilarating. "The fact that I don't know what I'll face every day is pure joy. I see new people and new things every day. And I am overjoyed by the different experiences I'm having — and humbled. I'm learning all the time."
CHA to provide resources on chaplain competencies, staffing
CHA is developing resources to guide Catholic health systems and facilities in determining how to appropriately staff their spiritual care departments and how to prioritize their chaplains' time, given the level of services the organizations wish to deliver.
CHA's pastoral care advisory committee has been working with representatives of several ministry organizations to create the resources. The group began by polling and talking with some CHA member organizations about the work of their chaplains. Using the results, the committee identified the top 15 essential services of chaplains.
The committee then created an online tool for ministry facilities to use to calculate how many chaplains they should have on staff to deliver various levels of spiritual care services. Users of the tool plug in information, including the number of annual adjusted patient days for their facility. The tool's algorithm calculates the number of chaplains the facility should have to provide spiritual care services at each of four different levels.
Several ministry organizations are piloting the tool and helping the committee to refine it. CHA expects to debut the resources, including the list of essential chaplain services and the staffing level calculator, within the next month. The resources will be available on the member section of the CHA website.
Carrie Meyer McGrath, CHA director of mission services, has been leading the project. She says the effort is in response to member requests for practical ways to implement the evolving standards and requirements put forth by the National Association of Catholic Chaplains and the Association of Professional Chaplains. Both are chaplain credentialing and education organizations.
— JULIE MINDA