By BETSY TAYLOR
Amber Baker delivered both her children by Cesarean section at PeaceHealth Southwest Medical Center in Vancouver, Wash. The birth of her first child, Keaton, she recalled as a blur. She had been in labor for 20 hours by the time she was wheeled into surgery. Staff checked Keaton's vital signs and handed him to his father while the surgeon closed Baker's incision. She didn't hold Keaton until she was in a recovery room.
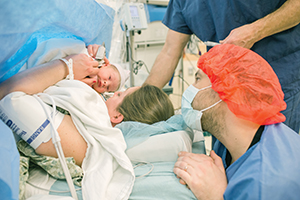
PeaceHealth Southwest Medical Center in Vancouver, Wash., made some changes to allow mothers like Amber Baker to have prompt skin-to-skin contact with their babies following most Cesarean births. Amber and her husband, Kody Baker, welcome their daughter, Cora, on Dec. 3.
When Baker was pregnant with her second child, she asked her obstetrician/gynecologist, Dr. Heather Weldon, to facilitate skin-to-skin contact between her and her newborn within the first few minutes of her baby's life outside the womb. A labor and delivery nurse at PeaceHealth Southwest Medical Center, Baker knew the physiological and psychological benefits of prompt and direct skin contact between mother and newborn.
When newborns at term are placed skin to skin with their mothers immediately following birth, several studies indicate the babies experience greater respiratory, temperature and glucose stability — a benefit that lasts for several hours. The contact promotes attachment between mother and child. Infants often exhibit the rooting instinct — finding and even latching on to a mother's breast during skin-to-skin contact, which facilitates breast-feeding. Research has shown fathers can also provide soothing and calming benefit to babies with skin-to-skin contact immediately following delivery.
Many U.S. hospitals support quick skin-to-skin contact when a woman delivers a baby vaginally. Increasingly, more U.S. hospitals are making changes to allow for skin-to-skin contact following Cesarean births. About one in three women in the U.S. deliver by C-section, according to the Centers for Disease Control and Prevention.
Weldon worked for a time in New Zealand. There, she said it was common for infants to get passed to the patient's midwife then directly to their mothers right after C-section delivery, provided neither mother nor babe required immediate medical attention. C-sections are usually done with a spinal or epidural anesthetic that doesn't affect the upper body. These moms are alert and able to safely hold their babies, Weldon said.

Weldon
Last year, when Weldon began as chair of the obstetrician/gynecology department at PeaceHealth Southwest Medical Center — a role that rotates among physicians — she worked to promote quick skin-to-skin contact following C-section deliveries.
Once delivered, babies remain attached to the umbilical cord for one minute to allow more blood to get to the baby, then the surgeon dries the baby so a receiving nurse can put the infant on a mother's chest after the cord is cut, Weldon explained. The mother can hold her child as her incision is closed.
At PeaceHealth Southwest, representatives from labor and delivery nursing, neonatal nursing, anesthesia, midwifery and obstetrics/gynecology met to determine the changes they'd need to make in order to facilitate skin-to-skin contact following C-section births. They worked out how to move the baby without compromising the sterile surgical field and how to position monitors to ensure there was room between a woman's head and chest for the baby to nest.
They planned for a nurse in each operating room to shift to a new role as a support person and observe the baby while the infant is being held by mom or dad in the surgery suite. The nurse conducts an Apgar test — assessing the baby's color, breathing effort, symptoms of pain and level of activity while the baby is skin to skin with the mom.
Weldon said emails were sent to obstetricians, anesthesiologists, nurses and midwives involved in deliveries outlining the changes. In huddles with nursing staff, charge nurses explained the changes and answered questions. In September, the medical center put the protocol in place. Weldon said it cannot always be used for unplanned C-sections, and it is not followed when a newborn or mother needs immediate medical attention.
Weldon said staff has modified its protocol and supply list based on experience. For example, surgical draping on the mother was too slippery to place a baby on, so they started using a different fabric. They switched to a neutral color draping to carry the baby from the surgical field to the mother's chest because the blue draping they had been using made it hard for those observing the infant to assess if the baby's color was healthy.
Baker said the changes don't create extra work for staff, and she now can personally attest to the benefits of skin-to-skin contact. She said it meant a great deal to hold her daughter, Cora, just a few minutes after her birth on Dec. 3. "It seems silly, but the baby just went from being in your belly, so the first place you want them to be is in your arms.
Copyright © 2017 by the Catholic Health Association
of the United States
For reprint permission, contact Betty Crosby or call (314) 253-3490.