By BETSY TAYLOR
Our Lady of Peace, a KentuckyOne Health behavioral health hospital and outpatient center in Louisville, opened a clinic in February to administer long-acting medication to help patients recovering from opioid or alcohol addictions reduce their cravings. The clinic also gives injections of long-acting psychiatric medications to patients with certain mental illnesses.
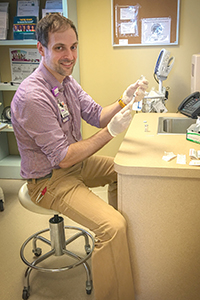
Clinical pharmacist specialist Robert Conzelman prepares an injection at the Our Lady of Peace retail pharmacy. The clinic within the behavioral health facility in Louisville, Ky., administers long-acting medications to outpatients with mental illness or recovering from addiction.
At the clinic — which operates as a retail pharmacy within Our Lady of Peace — a pharmacist dispenses and administers about a half dozen long-acting medications through injections. Each of the medications, prescribed by the patient's doctor, is administered roughly once a month. In the past, many of the opioid-addicted patients had to visit a clinic daily for oral medication to curb cravings. The psychiatric patients had to fill prescriptions and then take their daily doses of medication, something that some patients do not do for a variety of reasons.
Our Lady of Peace is a 220-bed behavioral health hospital with an average daily inpatient census of 90 adults and about 90 to 100 children and adolescents. About 50 patients at a time are detoxifying to remove alcohol or addictive drugs from their systems, explained Steve Cummings, Our Lady of Peace pharmacist. The hospital also provides partial hospitalization and intensive outpatient behavioral health services and runs a day hospital program.
Cummings said early response from the patients receiving injections from a pharmacist at the clinic has been positive, with some patients saying they were glad or grateful for the convenience. There are few clinics where outpatients can go for such injections.
Changing the model
Cummings said he championed the clinic because he saw a need for a new model for dispensing, administering and getting paid for the treatments. In the past, some patients returned to the hospital for an injection of their long-acting medication but Cummings said the hospital often had to absorb the cost.
The new model includes the addition of staff medication access coordinator Jasmine Douglas and clinical pharmacist specialist Robert Conzelman. Douglas determines if a patient's insurance formulary covers a particular medication and makes sure prior authorization criteria has been met to ensure payment for a medication. If a medication isn't covered by a patient's insurance and that patient has high out-of-pocket costs, Conzelman works with the patient's doctor to substitute a different brand of a generic drug or another effective medication. In other cases, Douglas reaches out to a drug company to see if the company has a program to lower or cover patient costs. Cummings said physicians appreciate that the new clinic is handling prior authorization paperwork related to processing prescriptions.
Reducing cravings
For opioid- or alcohol-addicted patients trying to stay substance-free, the clinic's pharmacist administers Vivitrol, the injectable, extended-release form of the drug naltrexone. According to the Substance Abuse and Mental Health Services Administration, naltrexone "blocks the euphoric and sedative effects of drugs like heroin, morphine or codeine. It binds and blocks opioid receptors" to reduce cravings. It also blocks the pleasurable effects of alcohol. Cummings said it is not a controlled substance.

Cummings
Ideally, an inpatient at Our Lady of Peace would begin the drug regimen before he or she is discharged, as soon as it's physically safe for the person to do so. Addicts must have no alcohol or narcotics in their system when they begin naltrexone injections, Cummings said.
People with schizoaffective disorder, who struggle to stay on daily medications, may be prescribed a long-acting injection medication. Cummings said the clinic can dispense and administer about a half dozen such medications. People with schizoaffective disorder experience psychotic symptoms, which may include hallucinations or delusions, and symptoms of a mood disorder, such as episodes of depression, or episodes of mania.
The clinic is open from 10 a.m. to 6:30 p.m. Monday through Thursday and from 7 a.m. to 3 p.m. on Fridays. It also offers immunizations to the public.
Cummings said, in order to have a manageable workload, the clinic's pharmacist administers a maximum of 20 to 25 shots a day.
An option, not a cure-all
"This isn't going to be for everybody," Cummings said. He said patients receiving the shots get them in conjunction with other treatment, such as individual mental health counseling and group therapy. Clinic staff check in with mental health providers to see if a person is attending therapy sessions. The pharmacist confers with a patient's doctor if a patient appears to be struggling when he or she comes in for an injection appointment, to see if treatment needs to be adjusted.
Cummings said a patient with a history of opioid abuse is given a small dose of oral naltrexone when the person arrives for each appointment. If the person shows signs of withdrawal within 30 minutes to an hour — an indication the person has not fully detoxed from opioids or has started using again — that individual won't be given the Vivitrol shot. The person can return to take the test another time and get the drug when he or she passes the challenge.
The number of times a patient receives a Vivitrol shot varies. For instance, some people experiencing alcohol cravings and worried about relapse may find that a few months of the shot helps them persevere until they are more confident in their sobriety. A person addicted to opioids may stay on Vivitrol longer, preferring the once-monthly shot to the need to visit a clinic daily for methadone. Methadone is an opioid used in medically assisted treatment to curb heroin or other opioid cravings.
Seeking solutions
Courtney Eatmon, a clinical pharmacist in Lexington, Ky., works with some patients who are taking the long-acting injectable medications in a hospital setting. She reached out to Our Lady of Peace to find out more about its clinic model.
She said there are benefits and risks associated with long-acting injectable medications. One particular concern occurs if someone on Vivitrol tries to use opioids. The person is at overdose risk if they're on Vivitrol, because they may take fatal quantities of opioids to attain pleasurable effects though the receptors that produce those effects have been blocked. Conversely, when people addicted to opioids stop taking Vivitrol, their tolerance to opioids will be greatly decreased, assuming they haven't been taking opioids, and they run a risk of overdose if they try to get high, particularly if they try to use opioids at the same dose they used to.
She said a person shouldn't consume alcohol when taking Vivitrol, but drinking alcohol while on the medication does not put a person at a heightened risk of death.
Jean Henry is the executive director of the National Alliance on Mental Illness—Louisville; she previously served in a director's role at Our Lady of Peace. She said putting the clinic at the behavioral health hospital makes sense, as many patients with addictions or mental health conditions know the location and know staff there.
She said, particularly for people who are noncompliant with daily medication dosing, an injectable psychotropic medication can provide a longer period of symptom management. Once stabilized, these patients may come to see the benefits of staying on their medication, she said.
Copyright © 2017 by the Catholic Health Association
of the United States
For reprint permission, contact Betty Crosby or call (314) 253-3490.