Collaborations include forward-thinking practicums, research, education, community service
By JULIE MINDA
Health care providers and nursing schools are developing shared programming that furthers their missions and meets community needs — especially the need to stem worsening nurse shortages.

Nursing students Becca Taylo, left, and Ashley Henkenius pose with a man they cared for at a foot-care clinic. Briar Cliff University in Sioux City periodically holds the free clinics at day shelters and sometimes does so in partnership with MercyOne's street medicine for the homeless program.
Catholic health care facilities are among those that have forged collaborations with their local nursing schools to create impactful programs that include research components, prepare students for the future of nursing practice and expose nurses to geriatric care and rural practices — sectors where nursing shortages are severe.
"There is no limit to the kinds of partnerships that health care organizations and nursing schools can create," says Polly Bednash, who was executive director of the American Association of Colleges of Nursing for nearly three decades and who now is a member of the CommonSpirit Health Board of Stewardship Trustees. (CommonSpirit is the Catholic system formed by the January merger of Catholic Health Initiatives and Dignity Health.)

Bednash
Shifting sands
Bednash says in the early history of health care in the U.S., people who aspired to be nurses would work in apprenticeships at hospitals. Eventually, many hospitals created their own internal nursing schools, and often their students would take additional coursework at local universities. Over time, many of these hospitals determined their nurses would need a more rigorous education in science than a single hospital could provide. The hospitals also recognized that their trained nurses were limited in career prospects — having earned a nursing certificate but not a degree. So many hospitals closed their nursing schools.
But, in closing the schools, "we often threw the baby out with the bathwater," says Bednash. A separation grew between the academic and clinical worlds of nursing. The American Association of Colleges of Nursing and other organizations recently have been encouraging partnership between health care facilities and nursing schools.
Bednash says much can be gained from coming together. Both schools and health care facilities "can enhance their work and gain a broader understanding of the needs of the community. … They can come together to meet those needs."
She says with the Catholic health ministry's propensity toward collaboration, it is well positioned to partner with nursing schools.
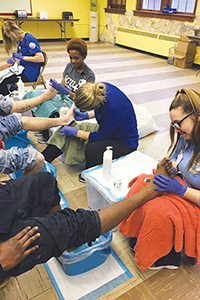
Briar Cliff University nursing students and a staff member examine feet at a clinic held in December at a warming shelter in Sioux City, Iowa. From left, are Kaitlin Pauls, Jolie Nkeshimana, Cathy Grimsley and Lyndsey Johnson. Grimsley is a program director with the university's nursing program.
Pipeline
Most collaborations are aimed at least in part at relieving the nurse workforce shortage. Nurses have been in short supply for decades, but prognosticators say the signs point to an even tighter labor market going forward. According to the American Association of Colleges of Nursing, "the shortage of registered nurses … is expected to intensify as baby boomers age and the need for health care grows. Compounding the problem is the fact that nursing schools across the country are struggling to expand capacity to meet the rising demand for care given the national move toward health care reform."
Mercy Hospital Ardmore in Ardmore, Okla., and Murray State College have teamed to address one aspect of the capacity issue by creating "Murray at Mercy." Mercy has converted outmoded ICU space on its campus into classroom space, two hospital room labs and a study lounge for students. The full-time, two-year program yields an associate degree in nursing. Students supplement their classroom learning and practicum time at the Mercy campus with college courses off-site.
Murray State Tishomingo faculty teach at Murray at Mercy. Murray at Mercy will hire two adjunct faculty in the program's second year — potentially Mercy staff. Murray is spending $270,000 over three years on Murray at Mercy, and the Mercy Foundation, more than $230,000, with the bulk of this funding going toward the adjunct faculty, the reconstruction of the space, furniture and supplies.

This graduate nursing class meets three times a semester on campus at The College of St. Scholastica in Duluth, Minn. The class members are family nurse practitioner students involved in a program that operates in partnership with Essentia Health –St. Mary's Medical Center of Duluth.
The inaugural class of 14 students started classes in January. Most have completed two semesters of science education before entering the program. Two of the students are Mercy respiratory therapists, and one a Mercy nurse aide.
Debbie Pender, vice president and chief nursing officer of Mercy Ardmore Communities, says she expects the program will help address nurse shortages, including by graduating all nurses in December, when the hospital has had problems finding recent graduates for open positions. Murray at Mercy will graduate its first class in December 2020.
Future workforce
Sheryl Sandahl is interim dean of nursing and a professor at The College of St. Scholastica in Duluth, Minn., a Catholic university that shares a Benedictine heritage with one of the hospitals it partners with, Essentia Health – St. Mary's Medical Center of Duluth. In recent years, Sandahl says, the university, the medical center and the medical center's parent, Essentia Health, have worked together on grant-funded programs to help prepare the nursing workforce for the future of health care delivery.
This includes curriculum and programming to expose nursing students to the ambulatory care environment and to equip them to practice preventive, holistic medicine. Another program places advance practice nursing students in rural settings and provides them with scholarships that incentivize them to practice in rural facilities after graduation.
Sandahl says of the work, "Health care is changing so quickly, and we're looking at how we can adapt."
Senior care
A collaboration on a Program of All-Inclusive Care for the Elderly in Philadelphia is reaping rewards for Trinity Health PACE and the University of Pennsylvania School of Nursing. That school founded the PACE site and turned it over to Trinity Health three years ago.
Trinity Health owns and staffs the PACE program, now known as Mercy LIFE West Philadelphia in affiliation with the University of Pennsylvania School of Nursing. The nursing school uses it as a practice site for nursing students — for practicums, shadowing, observation and volunteerism.
The nursing school partners with the PACE site to conduct on-site studies in areas impacting senior adults — everything from fall prevention to robot-assisted therapy. Nursing school faculty also provide education and support to Trinity PACE staff. Mercy LIFE, the nursing school and Trinity Health disseminate the educational resources and research findings to this and other Trinity Health PACE sites.

Hopkins
Kelly Hopkins, president and chief executive of Trinity Health PACE, says the collaboration gives students "valuable expertise working with seniors. We hope it helps the students develop a passion for the work, too — because we would love to see them choose careers serving elders after they graduate."

McElroy
Carrie Hays McElroy, vice president of clinical operations and chief nursing and compliance officer for Trinity Health PACE, says working with an academic partner to this degree is highly unusual for a PACE program, and it has brought an innovative flavor to the site's work.
Antonia Villarruel is a professor and the Margaret Bond Simon dean of nursing at the university. She says that since this is such a highly unusual collaboration, the school and health care partner have had to build trust with one another, and they've had to be creative in developing new models of working together.

Murray State College and Mercy Hospital Ardmore co-workers and leaders join in prayer before touring the "Murray at Mercy" nursing education space that opened at Mercy in January. The hospital is in Ardmore, Okla.
Community service
MercyOne of Sioux City, Iowa, sponsors a long-standing street medicine program that provides health care to people who are homeless. Since 2017 nursing students at the Franciscan Briar Cliff University of Sioux City have staffed 11 foot care clinics for people who are homeless. Many of the clinics are conducted in partnership with the street medicine team. All told, 46 students have gained experience examining 162 exceedingly vulnerable patients — a population that the students otherwise may never have encountered. At the clinics, nursing students wash and groom feet, assess feet for health concerns, and distribute new socks and shoes.
Cathy Grimsley, assistant professor and prelicensure BSN program director for Briar Cliff's Department of Nursing, says students who initially had been reticent about performing this particular brand of community service end up after the experience saying, "Wow, what an impact that had on me."
The foot clinics are important because foot assessments can flag serious health conditions. And, "the feet are the main mode of transportation for homeless people," Grimsley says.
She adds that through the foot clinics and other collaborations Briar Cliff and MercyOne have found a "natural fit. Our mission and values line up really easily."
Survey tool helps colleges, universities assess their engagement in social mission
An institute at George Washington University is offering a survey tool to dental, nursing and medical schools in the U.S. to enable them to measure engagement in social mission. As defined by the instrument, social mission has to do with addressing social determinants of health, increasing health equity and improving health outcomes for everyone.
The George Washington University Health Workforce Institute created the tool, called the Social Mission Metrics Study, with the support of the Robert Wood Johnson Foundation and the Health Resources and Service Administration's Bureau of Health Workforce. To create the study, the university's institute developed a questionnaire, field tested it with 60 schools and conducted four site visits to gather information on the experience of taking the survey.
Participating schools invite a multidisciplinary group of school leaders to complete the survey. The survey takes several hours to complete and includes questions related to the schools' mission, curriculum, extracurricular activities, global health work, response to community needs, community collaborations, student diversity, faculty diversity, academic leadership diversity, student training, faculty training, student activism, faculty activism, research, and other areas.
A research team from the institute analyzes and quantifies the responses, providing feedback. Participating schools can compare their performance against others and use the tool to track their social mission engagement over time.
Information on the Social Mission Metrics Initiative is available at https://socialmissionmetrics.gwhwi.org/. The site contains a webinar explaining the tool.
— JULIE MINDA
Partnerships help to build up nursing workforce
Among the ministry members that have found creative ways to partner with schools of nursing are:
- Avera St. Mary's Hospital, Pierre, S.D., which is providing funding for at least two academic years to sustain a University of South Dakota nursing program at the Capital University Center in Pierre. That center is a satellite location for six South Dakota public universities. Funding from Avera Health solidifies that program through the 2019-2020 academic year. The funding primarily will be used to offset the cost of employing faculty. (Avera is not disclosing its investment.) Avera may continue its contributions after 2020. Avera expects the funding to increase enrollment levels and so increase the number of new nurses in the job pool.
- Mercy College of Health Sciences, Des Moines, Iowa, a member of the MercyOne Catholic health system. The college has a four-year, $1.79 million grant from the Health Resources and Services Administration to increase the number of nursing students trained and working to the full scope of their licenses in primary care sites in Iowa.
- D'Youville Life and Wellness Community, Lowell, Mass., which collaborates with the University of Massachusetts Lowell School of Nursing to give the university's nursing students hands-on experience with eldercare. College juniors are paired with nurses at D'Youville's Center for Advanced Therapy for a seven-week rotation in gerontological rehabilitation nursing. Students discover an affinity for gerontological nursing as they learn to provide holistic care to frail seniors.
- Catholic Health of Buffalo, N.Y., which helped secure a grant of about $5 million from Community Partners of Western New York toward the development of a Health Professions Hub at D'Youville College of Buffalo. The clinical training center will provide learning opportunities for high school, undergraduate and graduate students — including those interested in nursing. Community members will be able to seek primary care at the hub's clinic. Catholic Health will provide staffing and resources for that clinic. The hub is to open in fall 2020.
- Catholic Health's Sisters of Charity Hospital of Buffalo and its partner, the University at Buffalo School of Nursing, which have received commendation from the American Association of Colleges of Nursing for their academic-practice partnership. The partnership involves clinical, research, education and professional development opportunities for the students and nurses. Students and nurse mentors work together in "dedicated education units" at the hospital.